Basic Thyroid Package Test Results
Following is a sample of the results of the Basic Thyroid Package blood test. The reference interval indicates the normal ranges and the flag indicates a result outside of those ranges. Both LabCorp and Quest Diagnostics measure T4 levels using micrograms per Liter for their reference ranges.
- The thyroid stimulating hormone or TSH signals the thyroid to perform its job and burn calories.
- Low TSH results may indicate hyperthyroidism.
- Elevated TSH results may indicate hypothyroidism.
- T3 uptake is used to estimate the amount of TBG (Thyroxine-Binding Globulin) in the blood and how much T3 and T4 is available for the body to use.
- T3 uptake directly affects the T3 and T4 levels.
- T4 circulates in the blood and influences how other organs and the heart function in the body.
-
- Elevated levels of T4 may indicate hyperthyroidism or thyroiditis. Abnormal elevated results may also be caused by too much iodine, high levels of protein in the blood, or too much thyroid medication.
- Low levels of T4 may indicate hypothyroidism, iodine deficiency, or possible pituitary gland disorder.
- T7 is a calculated measure of T4 x T3U (T3 Uptake)
LabCorp Example

TSH reference range: 0.450 to 4.500 uIU/mL. Thyroid Panel: Thyroxine (T4): reference range 4.5 to 12.0 ug/dL; T3 Uptake: 24-39%; Free Thyroxine Index (T7): 1.2 to 4.9.
Quest Diagnostics Example
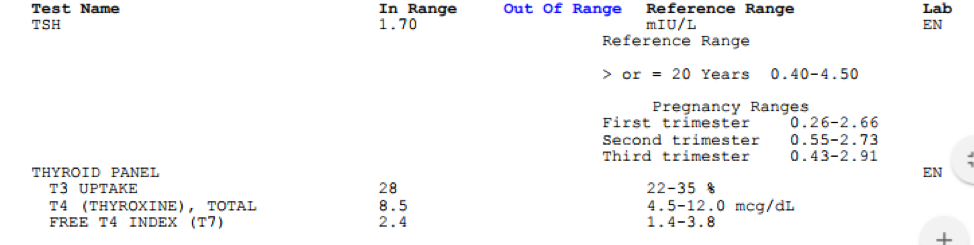
TSH reference range: Adults 20 years and older 0.450 to 4.500 uIU/mL Pregnancy reference ranges: Frist Trimester 0.26 to 2.66 mIU/L; Second Trimester 0.55 to 2.73 mIU/L; Third Trimester 0.43 to 2.91 mIU/L Thyroid Panel: Thyroxine (T4): reference range 4.5 to 12.0 mcg/dL; T3 Uptake: 22-35%; Free Thyroxine Index (T7): 1.4 to 3.8.
Expanded Thyroid Package Test Results
Following is a sample of the results of the Expanded Thyroid Package blood test. The reference interval indicates the normal ranges and the flag indicates a result outside of those ranges. Both LabCorp and Quest Diagnostics measure T4 levels using micrograms per Liter for their reference ranges.
- The thyroid stimulating hormone or TSH signals the thyroid to perform its job and burn calories.
- Low TSH results may indicate hyperthyroidism.
- Elevated TSH results may indicate hypothyroidism.
- T3 uptake is used to estimate the amount of TBG (Thyroxine-Binding Globulin) in the blood and how much T3 and T4 is available for the body to use.
- T3 uptake directly affects the T3 and T4 levels.
- T4 circulates in the blood and influences how other organs and the heart function in the body.
- Elevated levels of T4 may indicate hyperthyroidism or thyroiditis. Abnormal elevated results may also be caused by too much iodine, high levels of protein in the blood, or too much thyroid medication.
- Low levels of T4 may indicate hypothyroidism, iodine deficiency, or possible pituitary gland disorder.
- T7 is a calculated measure of T4 x T3U (T3 Uptake)
- Free T3 is used to help diagnose thyroid disorders, especially hyperthyroidism (overactive thyroid).
- Elevated Free T3 results may be an indicator of hyperthyroidism
- Low Free T3 result may be an indicator of hypothyroidism
- Free T4 is a hormone produced by the thyroid gland. T4 helps regulate metabolism and body temperature.
- Elevated Free T4 results may indicate hyperthyroidism.
- Low Free T4 results may indicate hypothyroidism.
LabCorp Example
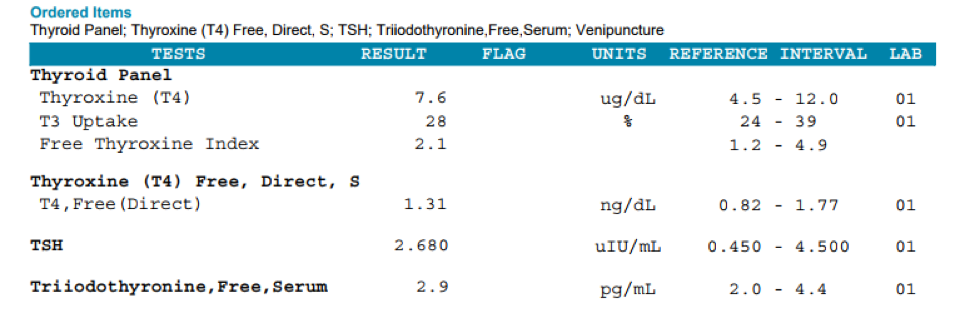
TSH reference range: 0.450 to 4.500 uIU/mL. Thyroid Panel: Thyroxine (T4): reference range 4.5 to 12.0 ug/dL; T3 Uptake: 24-39%; Free Thyroxine Index (T7): 1.2 to 4.9; Thyroxine T4 Free: reference range 0.82 to 1.77 ng/dL; Triiodothyronine (T3) Free: reference range 2.0 to 4.4 pg/mL.
Quest Diagnostics Example

TSH reference range: Adults 20 years and older 0.450 to 4.500 uIU/mL. Pregnancy reference ranges: Frist Trimester 0.26 to 2.66 mIU/L; Second Trimester 0.55 to 2.73 mIU/L; Third Trimester 0.43 to 2.91 mIU/L. Thyroid Panel: Thyroxine (T4): reference range 4.5 to 12.0 mcg/dL; T3 Uptake: 22-35%; Free Thyroxine Index (T7): 1.4 to 3.8; Thyroxine T4 Free: reference range 0.8 to 1.8 ng/dL; Triiodothyronine (T3) Free: reference range 2.3 to 4.2 pg/mL.
Thyroid Profile Test Results
Following is a sample of the results of the Thyroid Profile (T3T4T7) blood test. The reference interval indicates the normal ranges and the flag indicates a result outside of those ranges. Both LabCorp and Quest Diagnostics measure T4 levels using micrograms per Liter for their reference ranges. A Thyroid Profile (T3T4T7) blood test is a useful test for anyone suspecting thyroid problems. This blood test can help explain problems associated with fatigue, metabolism, and general feelings of ill health. The Thyroid Profile blood test is also used to monitor hormone levels for individuals that are taking thyroid supplements.
- T3 uptake is used to estimate the amount of TBG (Thyroxine-Binding Globulin) in the blood and how much T3 and T4 is available for the body to use.
- T3 uptake directly affects the T3 and T4 levels.
- T4 circulates in the blood and influences how other organs and the heart function in the body.
- Elevated levels of T4 may indicate hyperthyroidism or thyroiditis. Abnormal elevated results may also be caused by too much iodine, high levels of protein in the blood, or too much thyroid medication.
- Low levels of T4 may indicate hypothyroidism, iodine deficiency, or possible pituitary gland disorder.
- T7 is a calculated measure of T4 x T3U (T3 Uptake)
LabCorp Example

Thyroid Panel: Thyroxine (T4): reference range 4.5 to 12.0 ug/dL; T3 Uptake: 24-39%; Free Thyroxine Index (T7): 1.2 to 4.9.
Quest Diagnostics Example

Thyroid Panel: Thyroxine (T4): reference range 4.5 to 12.0 mcg/dL; T3 Uptake: 22-35%; Free Thyroxine Index (T7): 1.4 to 3.8.
Iodine Test Results
Following is a sample of the results of the Iodine blood test. The reference interval indicates the normal ranges and the flag indicates a result outside of those ranges. Too little or too much iodine in the blood may contribute to possible Thyroid conditions such as Hyperthyroidism or Hypothyroidism. Both LabCorp and Quest Diagnostics measure Iodine levels using micrograms per Liter for their reference ranges.
LabCorp Example

Iodine reference range: 40.0 to 92.0 ug/L. If your Iodine result is less than 20ug/L it will only show on the result as <20 ug/L.
Quest Diagnostics Example

Iodine reference range: 52 to 109 mcg/L.
Parathyroid Hormone () with Calcium Test Results
Following is a sample of the results of the PTH with Calcium blood test. The reference interval indicates the normal ranges and the flag indicates a result outside of those ranges. The Parathyroid helps regulate calcium levels. This test will provide valuable information as to how the Parathyroid is functioning.
- High levels of PTH with low calcium levels may be an indicator that the Parathyroid glands are functioning properly.
- Other tests such as Vitamin D, phosphorus and magnesium levels may be needed to determine if they are affecting your calcium levels.
- High levels of PTH with high calcium levels may be an indicator of hyperparathyroidism.
LabCorp Example
Calcium reference range: 8.7 to 10.2 mg/dL. PTH reference range: 15-65 pg/mL. The chart below the results may be used as a guideline for Interpretation of the PTH and Calcium results. Both the PTH and Calcium results are used for this interpretation.
Quest Diagnostics Example

Calcium reference range: 8.6 to 10.2 mg/dL. PTH reference range: 14-64 pg/mL. The chart between the results may be used as a guideline for Interpretation of the PTH and Calcium results. Both the PTH and Calcium results are used for this interpretation.
Parathyroid Hormone (PTH) Test Results
Following is a sample of the results of the PTH blood test. The reference interval indicates the normal ranges and the flag indicates a result outside of those ranges. The Parathyroid helps regulate calcium levels. This test will provide valuable information as to how the Parathyroid is functioning.
- High levels of PTH with low calcium levels may be an indicator that the Parathyroid glands are functioning properly.
- Other tests such as Vitamin D, phosphorus and magnesium levels may be needed to determine if they are affecting your calcium levels.
- High levels of PTH with high calcium levels may be an indicator of hyperparathyroidism.
LabCorp Example

PTH reference range: 15-65 pg/mL.
Quest Diagnostics Example
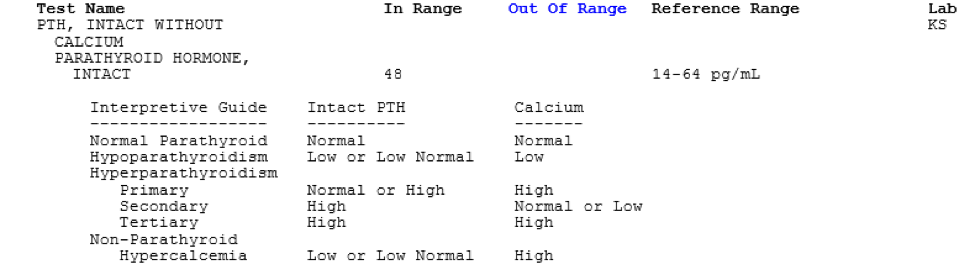
PTH reference range: 14-64 pg/mL. The chart below the result may be used as a guideline for interpretation of the PTH result.
Reverse Triiodothyronine (T3) Test Results
Following is a sample of the results of the Reverse T3 blood test. The reference interval indicates the normal ranges and the flag indicates a result outside of those ranges. Reverse T3 is the mirrored image of T3. Reverse T3 is the nonactive hormone where T3 is the active hormone.
- Reverse T3 can inhibit the action of the T3 hormone causing symptoms of hypothyroidism.
- Elevated Reverse T3 may be an indicator of hypothyroidism at a cellular level.
LabCorp Example

Reverse T3 reference range: 9.2 to 24.1 ng/dL.
Quest Diagnostics Example

Reverse T3 reference range: 8 to 25 ng/dL.
Free Triiodothyronine (T3) Test Results
Following are sample results of the Free T4 blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. Free triiodothyronine (free T3) tests may be used to help evaluate and asses thyroid function. It is primarily used evaluate for hyperthyroidism or to monitor current treatment for a thyroid condition. Free T3 and Total T3 tests are commonly ordered after a TSH blood test is found to be abnormal, especially if the Free T4 test is not elevated.
- Elevated Free T3 results may be an indicator of hyperthyroidism
- Low Free T3 result may be an indicator of hypothyroidism
LabCorp Example

Free T3 reference range: 2.0 to 4.4 pg/mL.
Quest Diagnostics Example

Free T3 reference range: 2.3 to 4.2 pg/mL.
Triiodothyronine (T3) Total Test Results
Following are sample results of the Total T3 blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. The Total T3 test is commonly ordered with other Thyroid tests such as TSH and T4 to obtain a larger picture as to how your thyroid is working.
- Elevated levels of T3 may indicate hyperthyroidism or Grave’s disease.
- Low levels of T3 may indicate hypothyroidism.
- Low T3 levels may also be caused by starvation, chronic illness or hospitalization.
LabCorp Example

Total T3 reference range: 71 to 180 ng/dL.
Quest Diagnostics Example

Total T3 reference range: 76 to 181 ng/dL.
Free Thyroxine (T4) Test Results
Following are sample results of the Free T4 blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. Free thyroxine (free T4) tests may be used to help evaluate and asses thyroid function for thyroid conditions such as hyperthyroidism and hypothyroidism. Free T4 tests are commonly ordered after a TSH blood test is found to be abnormal.
- Elevated Free T4 results may indicate hyperthyroidism.
- Low Free T4 results may indicate hypothyroidism.
LabCorp Example

Free T4 reference range: 0.82 to 1.77 ng/dL.
Quest Diagnostics Example

Free T4 reference range: 0.8 to 1.8 ng/dL.
Thyroglobulin Antibody Test Results
Following are sample results of the Thyroglobulin Antibody blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. The Thyroglobulin Antibody test (AntiThyroglobulin) may be used as a tumor marker and to evaluate treatment of thyroid cancer. The test may also be ordered when an individual has symptoms of hyperthyroidism. The test is useful in monitoring the effectiveness of treatment in individuals with Graves Disease, before and after surgical thyroid removal, and other thyroid cancer treatments. This test is commonly ordered with a TSH test.
- Elevated levels of the thyroglobulin antibodies may indicate Graves disease or thyroiditis.
- Decreasing levels of thyroglobulin antibodies in individuals treated for Graves disease, indicates a response to the treatment.
LabCorp Example

Thyroglobulin Antibody reference range: 0.0 to 0.9 IU/mL.
Quest Diagnostics Example
![]()
Thyroglobulin Antibody reference range: < or = 1 IU/mL.
Thyroid Peroxidase (TPO) Antibodies Test Results
Following are sample results of the Thyroid Peroxidase Antibody (TPO) blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. The TPO antibody test is the most common test for autoimmune thyroid disease; it can be detected in Graves disease or Hashimoto thyroiditis.
- Elevated TPO results may indicate a thyroid autoimmune disorder such as Graves disease or Hashimoto thyroiditis.
- Elevated TPO levels may also indicate possible thyroid cancer or other autoimmune disease.
LabCorp Example

Thyroid Peroxidase Antibodies reference range: 0 to 34 IU/mL.
Quest Diagnostics Example

Thyroid Peroxidase Antibodies reference range: <9 IU/mL.
Thyroid Stimulating Immunoglobulin (TSI) Test Results
Following are sample results of the Thyroid Stimulating Immunoglobulin (TSI) blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges.
- High levels of TSI in the blood can indicate the presence of Graves’ disease, which is an autoimmune disorder that affects the thyroid gland. Grave’s disease may lead to or be the cause of hyperthyroidism.
- TSI levels may also reveal other thyroid disorders such as Hashimoto’s, which is one of the most common causes of hypothyroidism.
LabCorp Example

Thyroid Stimulating Immunoglobulin reference range: 0 to 139.
Thyroid-Stimulating Hormone () Test Results
Following are sample results of the Thyroid Stimulating Hormone (TSH) blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. A TSH blood test is commonly ordered when thyroid problems are suspected. Possible indications of thyroid problems may include weight loss, weight gain, feelings of extreme hot or cold, tiredness, rapid heart rate and irregular menstrual cycles.
- Low levels of TSH in the blood may indicate an overactive thyroid gland, thyroid gland, commonly referred to as hyperthyroidism.
- High levels of TSH in the blood may indicate an underactive thyroid gland, commonly referred to as hypothyroidism.
LabCorp Example
Thyroid Stimulating Hormone reference range: 0.450 to 4.500 uIU/L.
Quest Diagnostics Example

Thyroid Stimulating Hormone reference range: , adults 20 years and older 0.450 to 4.500 uIU/mL. Pregnancy reference ranges: Frist Trimester 0.26 to 2.66 mIU/L; Second Trimester 0.55 to 2.73 mIU/L; Third Trimester 0.43 to 2.91 mIU/L.
Thyroxine (T4) Total Test Results
Following are sample results of the Total T4 blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. Both LabCorp and Quest Diagnostics measure T4 levels using micrograms per Liter for their reference ranges.
- Elevated levels of T4 may indicate hyperthyroidism or thyroiditis. Abnormal elevated results may also be caused by too much iodine, high levels of protein in the blood, or too much thyroid medication.
- Low levels of T4 may indicate hypothyroidism, iodine deficiency, or possible pituitary gland disorder.
LabCorp Example

Total T4 reference range: 4.5 to 12.0 ug/dL.
Quest Diagnostics Example

Total T4 reference range: 4.5 to 12.0 mcg/dL.
TSH and Free T4 Test Results
Following are sample results of the TSH and Free T4 blood test. The reference intervals indicate the normal ranges and the flag indicates a result outside of those ranges. A TSH blood test is commonly ordered when thyroid problems are suspected. Free thyroxine (free T4) tests may be used to help evaluate and asses thyroid function for thyroid conditions such as hyperthyroidism and hypothyroidism.
- Low levels of TSH in the blood may indicate an overactive thyroid gland, thyroid gland, commonly referred to as hyperthyroidism.
- High levels of TSH in the blood may indicate an underactive thyroid gland, commonly referred to as hypothyroidism.
- Elevated Free T4 results may indicate hyperthyroidism.
- Low Free T4 results may indicate hypothyroidism.
LabCorp Example

TSH reference range: 0.450 to 4.500 uIU/mL. Free T4 (Direct): reference range .093 to 1.60 ng/dL.
Quest Diagnostics Example

TSH reference range: 0.40 to 4.50 mIU/L. Free T4 reference range: 0.8 to 1.8 ng/dL.


