Everything You Need To Know About Blood Types
No matter your health status or your stage of life, understanding your blood type is essential. After all, your blood type isn’t necessarily identical to that of your partner, your parents, or your children. You and your loved ones could each have one of eight different blood types, each of which contain antigens that may make it incompatible with others.
Fortunately, a simple test can indicate your blood type, revealing clues about your health, providing critical information before a medical procedure, and even telling you how valuable you are as a blood donor. Find out how blood typing works, learn why this process is critical, and discover the vast array of information you can learn from a blood type test.
How Antigens Determine Your Blood Type
No matter your type, all blood contains the same basic building blocks. Blood includes red blood cells that transport oxygen, white blood cells that combat infections, and platelets that aid in clotting when you’re injured. Plasma, a fluid that consists of proteins and salts, carries all blood cells through your veins.
Your antigen makeup is the key factor in determining your blood type. Antigens reside on the surface of your red blood cells, where they serve as built-in protection devices for your blood supply. These substances are designed to identify foreign cells and trigger immune responses that produce antibodies in the plasma to attack potential invaders.
The presence or absence of antigens on your red blood cells and corresponding antibodies in your plasma defines your ABO blood group. This blood grouping system has four types:
- Group A: This blood group has A antigens and B antibodies.
- Group B: This blood group has B antigens and A antibodies.
- Group AB: This blood group has A and B antigens and no antibodies.
- Group O: This group doesn’t have either A or B antigens, but it has both A and B antibodies.
This blood group system may seem straightforward, but it’s still relatively new. In fact, Austrian physician Karl Landsteiner discovered the existence of antibodies and antigens in blood just over a century ago, in 1901. His work later led to the creation of blood groups, earned him a Nobel Prize in 1930, and contributed to significant advances in medicine.
The Rhesus System and Your Blood Type
A decade after receiving his Nobel Prize, Landsteiner and colleague A.S. Weiner discovered a secondary protein that also has a major impact on blood type. Their work with rhesus monkeys led to the creation of the Rhesus system, which highlights the presence or absence of the Rh factor.
If your red blood cells have this protein, your plasma naturally contains Rh antigens. That means you’re considered positive, or Rh+. If you don’t have this protein, your blood is considered Rh-, or negative.
Standard blood typing combines the ABO system with the Rhesus system to create a more complete picture of your blood profile. That means you could have one of eight blood types:
- Type A+: Contains A and Rh antigens as well as B antibodies.
- Type A-: Contains A antigens as well as B antibodies.
- Type B+: Contains B and Rh antigens as well as A antibodies.
- Type B-: Contains B antigens as well as A antibodies.
- Type AB+: Contains A, B, and Rh antigens but no antibodies.
- Type AB-: Contains A and B antigens.
- Type O+: Contains Rh antigens as well as A and B antibodies.
- Type O-: Contains no antigens but has A and B antibodies.
Although most people have one of the eight common blood types, some people don’t fit neatly into this standard system. Over 600 other antigens can reside on red blood cells, leading to countless rare blood types. Since blood type is hereditary, rare blood types typically exist in ethnic groups.
Why Blood Typing Is Important
Each blood type contains a delicate balance of antigens and antibodies, and not all blood types are compatible with one another. Since antibodies are designed to fight corresponding antigens, a transfusion that mixes two incompatible blood types could cause the antibodies in one to attack the antigens in another. These antibody attacks can lead to agglutination, or the creation of clumps of red blood cells. Agglutination can create clogs, stop circulation, and may cause red blood cells to split and leak, which triggers toxic reactions.
Since mixing incompatible types can be harmful or even fatal, understanding your blood type is critical, especially if you’re donating blood or receiving a transfusion from a donor. After all, some blood types can’t pair safely with others, while others are compatible with several other types. The eight standard blood groups can pair as follows:
- Type A+: Can donate blood to types A+ and AB+. Can receive blood donations from types A+, A-, O+, and O-.
- Type A-: Can donate blood to types A+, A-, AB+, and AB-. Can receive blood donations from types A- and O-.
- Type B+: Can donate blood to types B+ and AB+. Can receive blood donations from types B+, B-, O+, and O-.
- Type B-: Can donate blood to types B+, B-, AB+, and AB-. Can receive blood donations from types B- and O-.
- Type AB+: Can donate blood to type AB+. Can receive blood donations from all eight types.
- Type AB-: Can donate blood to types AB+ and AB-. Can receive blood donations from types AB-, A-, B-, and O-.
- Type O+: Can donate blood to types O+, A+, B+, and AB+. Can receive blood donations from types O+ and O-.
- Type O-: Can donate blood to all eight types. Can receive blood donations only from type O-.
Overall, types O+ and A+ are by far the most common blood types in the United States, appearing in 37 and 36 percent of the population, respectively. Almost 9% of Americans have either type B+ or O- blood, while 6% have type A-, and 3% have type AB+ blood. Types B- and AB- are the least common in the U.S., appearing in 2% and less than 1% of the population, respectively.
What Your Blood Type May Tell You
While blood typing is essential before a transfusion or a donation, understanding your blood type can also reveal much more about you. Knowing your blood type can help you learn about your history and genetic makeup as well as your risk factors for developing serious health issues in the future.
Since each blood type appears in varying frequencies across the globe, understanding your blood type could help you pinpoint your ancestors. For example, blood type Rh+ is very common across the globe. It tends to appear most frequently in Asia and Australia, but Western Europeans and those with Basque heritage have some of the highest frequencies of blood type Rh-.
In addition, blood type A appears frequently in all populations, but it’s most predominant in North America and Europe. Blood type O is also common around the world, but it appears most frequently in Central and South America. In contrast, blood type B is relatively uncommon outside of Central Asia, Northern India, and Russia.
In many cases, your blood type can also shed light on diseases to which you may be more susceptible, as well as health conditions to which your body may be more resistant. After all, type A is the oldest of the ABO blood groups, while types O and B appeared much later. Like most genetic mutations, blood types O and B gave bearers select advantages, including resistance to certain diseases.
While few studies have demonstrated clear links between blood type and risk factor for diseases, several reports have suggested connections between the two. For example, people with blood type AB tend to have higher levels of a protein that encourages blood clotting and may lead to strokes. Along the same lines, studies have shown that people with type A and type B blood have a greater chance of developing type 2 diabetes.
In contrast, those with blood type O tend to have a greater resistance to many serious diseases. Several studies have demonstrated that those with blood type O have a natural protection against one of the most harmful forms of malaria, while tests have also shown that those with blood type O also have a significantly reduced risk of developing stomach cancer. Studies have also shown that people with blood type O have the lowest risk of developing cardiovascular disease, suggesting that they may have naturally low levels of inflammation and low-density lipoprotein (LDL) cholesterol.
Why Your Blood Type Is Important in Pregnancy
Knowing your blood type can tell you more about yourself and potential health risks, and it’s also important if you’re planning to have a child. Finding out the blood type for the father, mother, and child is essential, as incompatible Rh factors can pose serious health risks for the mother as well as for future children.
If you and your baby have the same Rh factor, your blood types are considered compatible and won’t cause problems. However, if you have a negative Rh factor and your partner has a positive Rh factor, there’s a chance your baby has a negative Rh factor, which could lead to complications. While your blood won’t normally come into contact with your baby’s blood, the two could mix during delivery or if trauma occurs at any time during your pregnancy.
In the event that they do mix, your red blood cells could begin to produce Rh antibodies. While these antibodies aren’t likely to cause harm to you or your baby right away, they could affect your next child. During your next pregnancy, there’s a chance that the Rh antibodies could enter your baby’s blood supply. If you’re Rh- and your baby is Rh+, the antibodies could attack your baby’s red blood cells and cause anemia, a condition that could be fatal to your unborn child.
To combat these potential complications, physicians often recommend that Rh- mothers have a blood test to screen for antibodies during the first trimester and again at delivery. If you test positive for Rh antibodies at your 28th week of pregnancy, your obstetrician will generally monitor you and your baby carefully, providing a blood transfusion for the baby if necessary.
If the antibody test you take in your first trimester produces a negative result, you’ll typically receive an Rh immune globulin injection to prevent your blood cells from generating any antibodies throughout your pregnancy. You’ll undergo another blood test at delivery. If your baby is born Rh+, you’ll typically need a second injection, but if your baby is born Rh-, you won’t usually need additional treatment.
In some cases, you’ll need additional injections to protect yourself and any future children. Prenatal tests like amniocentesis, chorionic villus sampling, or cordocentesis can all cause your baby’s blood to mix with yours and may require an injection. If you experience a miscarriage, an ectopic pregnancy, substantial bleeding, or an abortion, Rh immune globulin is typically necessary.
What Influences Your Blood Type
Blood type is a hereditary trait, as parents’ blood types determine their children’s. While children’s blood types aren’t necessarily an exact match for one of their parents, understanding parents’ blood types can help narrow down the potential types that children could have.
A single gene determines ABO blood type, and three versions of the gene exist: A, B, and O. Both A and B versions of the blood type gene are dominant, and the O version is recessive. Children inherit one version of the gene from each parent, resulting in six potential combinations of genes that place them in one of four ABO groups.
For example, a child who inherits an A version of the gene from one parent and a B version from the other will have blood type AB. Inheriting an A version and an O version of the gene will result in blood type A, while inheriting two O versions of the gene will result in blood type O.
A separate gene determines whether children have the Rh factor. Since Rh factor is either positive or negative, only two versions of this gene exist. In this case, the positive version is dominant, and the negative version is recessive. That means inheriting a positive version and a negative version of the gene will result in blood type Rh+, while inheriting two negative versions will result in blood type Rh-.
Although creating a hereditary chart can help in assessing potential blood type options for current and future generations, this method isn’t scientific. Only a reliable test can confirm your blood type.
How Blood Typing Is Done
To find out your blood type, you’ll need to provide a blood sample. To begin the process, a clinician will sanitize your skin, ensure that your veins are visible, and then use a needle to draw a blood sample. The clinician will then place gauze over the puncture area and proceed with testing.
To complete the blood type test, the clinician will divide your sample into separate vials. The clinician will then mix your sample with a solution that contains A and B antibodies. If your blood cells react by forming clumps, then your blood contains at least one of the antigens. Next, the clinician will mix your plasma with either type A or type B blood to determine whether your blood has A, B, or both antibodies. Finally, the clinician will use a similar process of mixing your blood cells and plasma with Rh+ blood to determine your Rh factor.
After this test, you’ll know both your Rh factor and your ABO blood group, revealing your blood type. Since most blood type tests take mere minutes and the risks are minimal, blood typing is a simple and inexpensive process that can be incredibly informative.
What Happens If Your Blood Type Is Unknown
If you experience a medical emergency, it isn’t always possible to communicate your blood type, especially if you’re unconscious or in shock. Emergency medical technicians (EMTs) may not have time to perform a blood test before administering a transfusion, but that lack of information won’t typically delay emergency procedures or prevent you from getting the blood supply you need.
Long considered a universal blood type, O- blood tends to be compatible with all other standard blood types. In an emergency or if your life is in danger, medical personnel will most commonly administer O- blood.
Despite its reputation as a universal option, however, even O- blood may have antibodies that react with other types. Not everyone has one of the eight common blood types, but you won’t usually know this until you experience a medical emergency. Since even O- blood can cause complications that increase the risk of the transfusion, medical personnel typically strive to use blood that precisely matches that of the patient.
Whether you receive O- blood or your exact match, physicians generally begin the transfusion process by testing compatibility. Carefully cross-matching a small sample of your blood with the donor’s blood ensures that the two are compatible and won’t cause additional complications.
Blood Type and Organ Donation
If you need a new organ or you want to donate an organ, blood type testing can help assess your eligibility. The kidney donation process begins with blood typing, which determines the types of recipients who are compatible with you. Donors and recipients typically match as follows:
- Type A: Donors are compatible with type A and AB recipients.
- Type B: Donors are compatible with type B and AB recipients.
- Type AB: Donors are compatible with type AB recipients.
- Type O: Donors are compatible with all recipients.
Next, both the donor and the recipient undergo tissue typing, which compares 12 antigens to determine how compatible the tissue types are. While identical twins, siblings, parents, and children have the best chances of matching, even complete strangers can have few or even zero mismatches.
Both patients also undergo a second tissue type test that checks for antibodies that may attack the tissue. Since antibody levels can change over time, most transplant recipients complete frequent tests for months after surgery.
In most cases, close relatives and exact blood type matches are ideal and increase the chances of success from an organ donation. However, antibody treatments may allow recipients to receive organs from donors without compatible blood types, ultimately increasing the range of donors available to a recipient in need of a transplant.
Blood Type and Donation Needs
From sickle cell patients who need recurring blood transfusions throughout their lives and cancer patients who require blood during a series of chemotherapy treatments to victims of car accidents who need large amounts of blood urgently, someone in the U.S. needs a blood donation every two seconds.
Although nearly seven million U.S. residents donate blood every year, less than 10% of people eligible to donate do so. Since red blood cells expire within six weeks of donation and platelets expire in just five days, blood donations are in constant demand across the nation.
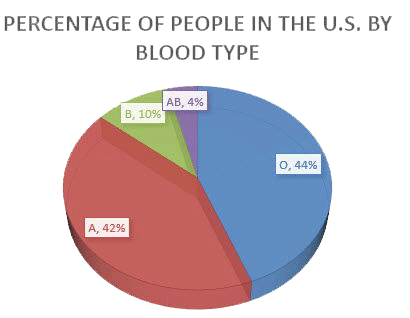
While red blood cells are in greatest demand, many patients need plasma and platelets, too. Since blood type O is compatible with the widest variety of blood types, it tends to be most frequently requested. Although almost half of Americans have type O blood, type O- is one of the least common among U.S. residents.
That means this highly compatible blood type tends to be in short supply. Fortunately, giving blood is relatively simple for eligible donors who can give whole blood every eight weeks. Because a single donation can save up to three lives, giving blood can have a substantial impact, no matter what your blood type.
Whether you want to prepare for a potential medical emergency, understand how your blood type could impact future children, assess your risk level for certain diseases, or learn more about hereditary factors, your blood type has the answers.
Knowing Your Blood Type
Many people understand that knowing your blood type is important in the event you need a blood transfusion. But it can also be important in other health scenarios.
Common Questions About Blood Types
Blood Type Facts And Donation
Everyone, regardless of age, gender or ethnicity, relies on blood to survive. As a result there is a constant need for all blood types. The available supply of blood is dependent on donations made by eligible individuals throughout the country. There is however, often a fear that is associated with the act of donating blood. Education is the best way to promote blood donation, overcome any fears about the process and help maintain the blood supply at a level that meets the current need.
The ABO Blood Group System
- Blood is categorized in four primary types, or groups, based off of the ABO system. The four potential blood types are A, B, AB, and O.
- Antigens that are on the surface of red blood cells are either type A or they are type B. Their presence, or absence, determines whether blood is a type A or B. Blood groups are determined based on these antigens.
- Blood types must be accurately matched for a safe red blood cell transfusion. People with type O blood can donate to all blood types and people with type A blood can donate to people with type A and type AB. A person with type B blood can safely donate to people with type B and type AB. If a person has type AB blood, he may donate red cells only to others with type AB.
- The presence of the Rh protein, or factor, in blood also helps determine a person’s blood type. The Rh factor is another type of antigen that may or may not be present in the blood. If it is present, the blood type is positive. If the Rh protein is absent, it is negative.
- Type O negative blood is the universal red cell donor. This means that a person that is O negative can donate his blood to anyone regardless of that person’s blood type. Type AB positive is the universal plasma donor. This means that a person with this blood type can donate blood to anyone.
What Happens to Donated Blood?
Step One: The Donation Process
- The donor completes the registration process.
- The donor provides a medical history and undergoes a mini physical examination.
- Blood is donated. The Red Cross collects several test tubes and one pint of blood from the donor.
- Identical barcoded labels are placed on the donor’s record, the bag and test tubes of blood.
- The donated blood is placed in coolers of ice where it is kept until it is taken to the Red Cross Center.
Step Two: Processing Procedure
- The test tubes are sent to be tested.
- The Red Cross scans the blood donation into its database.
- The donated blood is placed in a centrifuge and spun to separate the transfusable components.
- The Red Cross then leukocyte-reduces the red cells.
- Platelets are also leukocyte-reduced and they are bacterially tested.
Step Three: Testing Process
- There are five Red Cross National Testing Laboratories. The test tubes are sent to and then received by one of these laboratories.
- Each unit of blood undergoes a dozen tests. These tests are checking for infectious diseases and are meant to establish the blood type.
- Within 24 hours, results of the tests are electronically sent to the manufacturing facility.
- The donor is notified if the tests return positive for infectious diseases. The donated blood is discarded.
- The testing in this step occurs at the same time as Step two.
Step Four and Five: Storage and Distribution
- Labels are placed on units of blood that undergone testing and are found to be safe.
- Refrigerators that are kept at six degrees Celsius are used for storing red cells. Red cells are stored for 42 days only.
- Agitators are used to store platelets at room temperature. They are kept for no longer than five days.
- Freezers are used to freeze and store plasma and cryo for one year.
- Shipping of blood can occur at any time, seven days a week and at any hour.
Sources
Stanford Blood Center. Blood Types. Last accessed February 10, 2023. https://stanfordbloodcenter.org/donate-blood/blood-donation-facts/blood-types/
American Red Cross. Importance of the Blood Supply. Last accessed February 10, 2023. https://www.redcrossblood.org/donate-blood/how-to-donate/how-blood-donations-help/blood-needs-blood-supply.html
American Red Cross. Facts About Blood and Blood Types. Last accessed February 10, 2023. https://www.redcrossblood.org/donate-blood/blood-types.html?icid=rdrt-blood-types&imed=direct&isource=drupal
ThermoFisher Scientific. Introduction to Immunoglobulins. Last accessed February 10, 2023. https://www.thermofisher.com/us/en/home/life-science/antibodies/antibodies-learning-center/antibodies-resource-library/antibody-methods/introduction-immunoglobulins.html
